Written by Varsha Meghnani, PhD, ASCP, NRCC.
Abstract:
The COVID-19 pandemic, caused by the SARS-CoV-2 virus, has led to more than 70 million confirmed cases, with over 1.6 million deaths globally. The virus which is believed to be originated from the Seafood market in Wuhan, China has now spread worldwide due to its high transmission rate [1]. To minimize the spread of the virus, countries around the globe have taken strict measures to maintain social distancing. The lockdown measures have not only disrupted people’s lives all over the world but also adversely affected the economies of many countries. Another crucial step taken by the countries is testing, identifying, and segregating the infected population from the rest of the healthy population. The tricky part is identifying those who are infected but show no symptoms i.e. Asymptomatic carriers. Such a population is often neglected as they are less likely to go to a doctor and get tested which makes it difficult to keep them away from the healthy population. Due to this, there is a need for a better pandemic management plan for controlling the spread of SARS-Cov-2.
Transmission:
The most crucial step in combating the spread of the pandemic is to understand the mechanism and rate of transmission. The following modes of transmission have been proposed by scientists.
Droplet transmission: Transmission occurs when a healthy person is in close contact with another person experiencing COVID-19 symptoms like coughing, sneezing, etc. The potentially infective respiratory droplets (5-10 µm) [2] from the infected persons’ cough and sneeze can transmit the infection to the surrounding healthy individual(s).
Airborne transmission: Airborne transmission happens in a similar fashion as Droplet transmission but the droplet size is <5μm in diameter and is often called droplet nuclei. These tiny particles can remain suspended in the air for longer periods of time and can be transmitted to others over a longer distance (more than 2 meters) [2].
Surface transmission: Surface transmission was initially considered a big contributor to the spread of the virus, but recent research studies have proposed that the chance of transmission through inanimate surfaces is very low.
This implies that a well-ventilated area poses a lower risk than the enclosed spaces with poor ventilation. Hence the transmission rate varies from one location to another. Transmission rate measures the reproduction rate of the virus and assesses the possible secondary infections from a single infection in a specific area. [3].
It is clear that social distancing is one of the most essential tools to reduce the spread of the virus, but it is not always feasible. Also identifying those who are infected but show no symptoms i.e. Asymptomatic carriers is difficult. Such a population is less likely to go to a doctor and get tested which makes it difficult to keep them away from the healthy population.
Asymptomatic carriers:
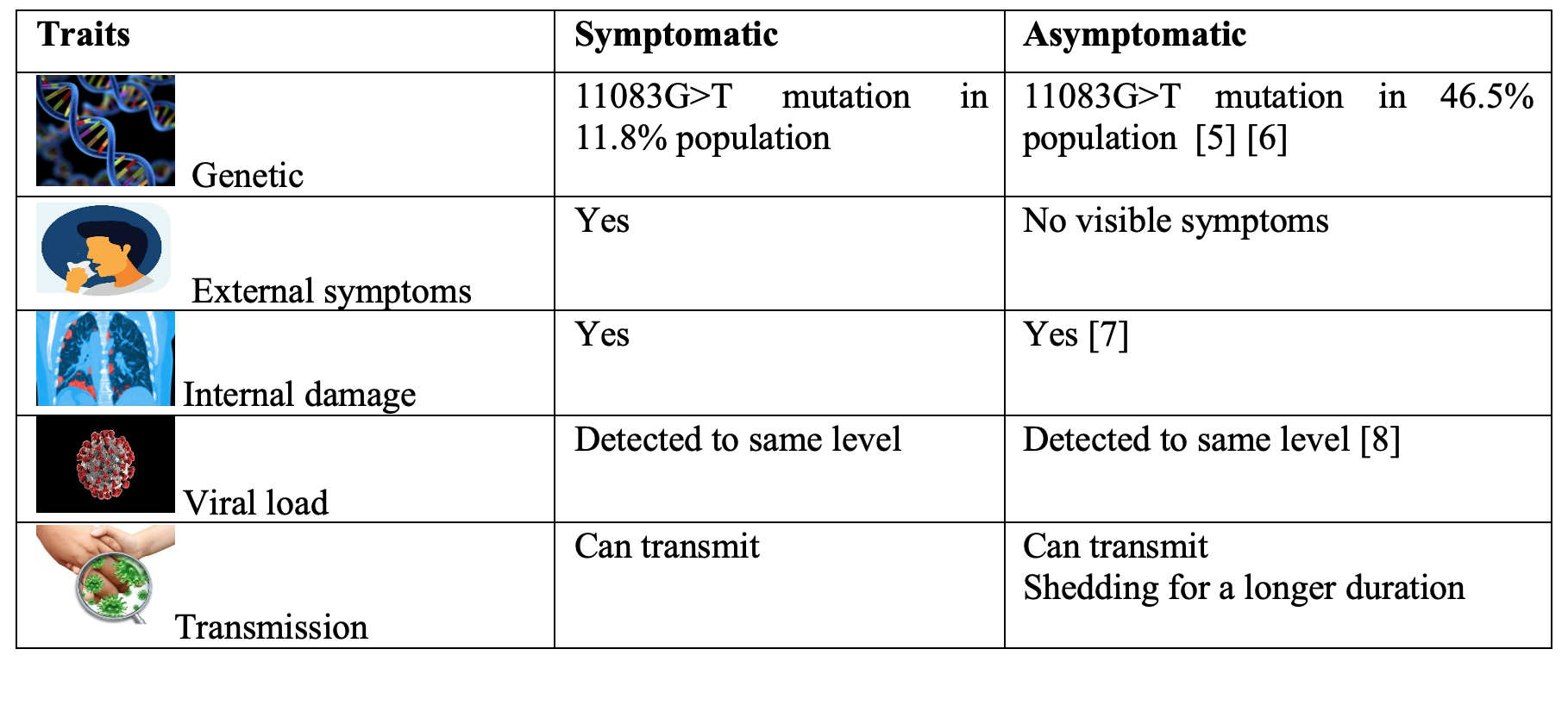
Studies have shown that about 30-40% population tested positive for SARS-Cov-2 virus never develop any obvious symptoms [4]. They do not get a fever, cough, cold, and shortness of breath. Research has revealed that asymptomatic infection might be linked to SARS-CoV-2 11083G>T mutation at nonstructure protein 6 of the virus. It is found that this mutation is more likely to be present in the asymptomatic population than their symptomatic counterparts. This is the first genomic level distinction between the symptomatic and asymptomatic population [5] [6]. Although the asymptomatic carriers are silent without symptoms but internally, they have shown signs of damage in their lungs and heart [7]. It is still not clear whether the damage is short-term or chronic.
Some misconceptions around the asymptomatic carriers are that they are less likely to spread the infection as they have less viral load than the symptomatic population. But, studies have shown similar viral loads in both asymptomatic as well as in symptomatic patients suggesting that people without symptoms have the ability to transmit the virus to others [8].
Since asymptomatic carriers don’t cough and/or sneeze, it is sometimes believed that they don’t spread the droplets/aerosols of the infection. But the research studies have shown that in comparison to symptomatic patients, the asymptomatic group had a significantly longer duration of viral shedding, with a viral shedding time of up to 19 days [8]. Several factors might contribute to the variation of the duration of viral shedding. One reason could be that patients with symptoms of SARS-CoV-2 infection are mostly admitted to hospital and receive proper treatment. However, asymptomatic individuals may not seek treatment and hence they shed the viral particles for a longer duration than the symptomatic patients.
Table 1. Similarities and differences between Symptomatic and Asymptomatic SARS-Cov-2 infection.
Diagnostic tests for COVID-19:
There is a wide range of tests available in the market for diagnosing the COVID-19 infections and for monitoring the recovery. The tests are divided into two major categories:
1. Molecular test: Molecular tests are based on their ability to detect the small amount of viral RNA in a sample. RT-PCR is the most commonly used molecular method and considered the gold standard technique for detection of the virus. A RT PCR positive result means that the individual is infected with the COVID-19 virus. A negative result may mean that the individual is not infected, is infected but is too early to be detected due to intermittent shedding, infected but has recovered, or a false negative. The method is being widely used to diagnose not only the symptomatic patients but also for screening the asymptomatic population. Recently some studies have published cases of false-negative RT PCR results for an asymptomatic population which was later confirmed by the serological tests. Such a data imply RT PCR alone is not enough for the detecting the virus in asymptomatic population [9].
2. Serological test: While RT-PCR-based viral RNA detection has been widely used in the diagnosis of COVID-19, it cannot be used to monitor the progress of the disease stages and to identify the past infection and immunity. Serological assays detect the presence of immunoglobulin M (IgM) and immunoglobulin G (IgG) antibodies against the virus in saliva, sputum, and other biological fluids. IgM is an indicator of early-stage infection as it is detectable in serum within a few days and lasts a couple of weeks upon infection. IgG is an indicator of current or prior infection [9].
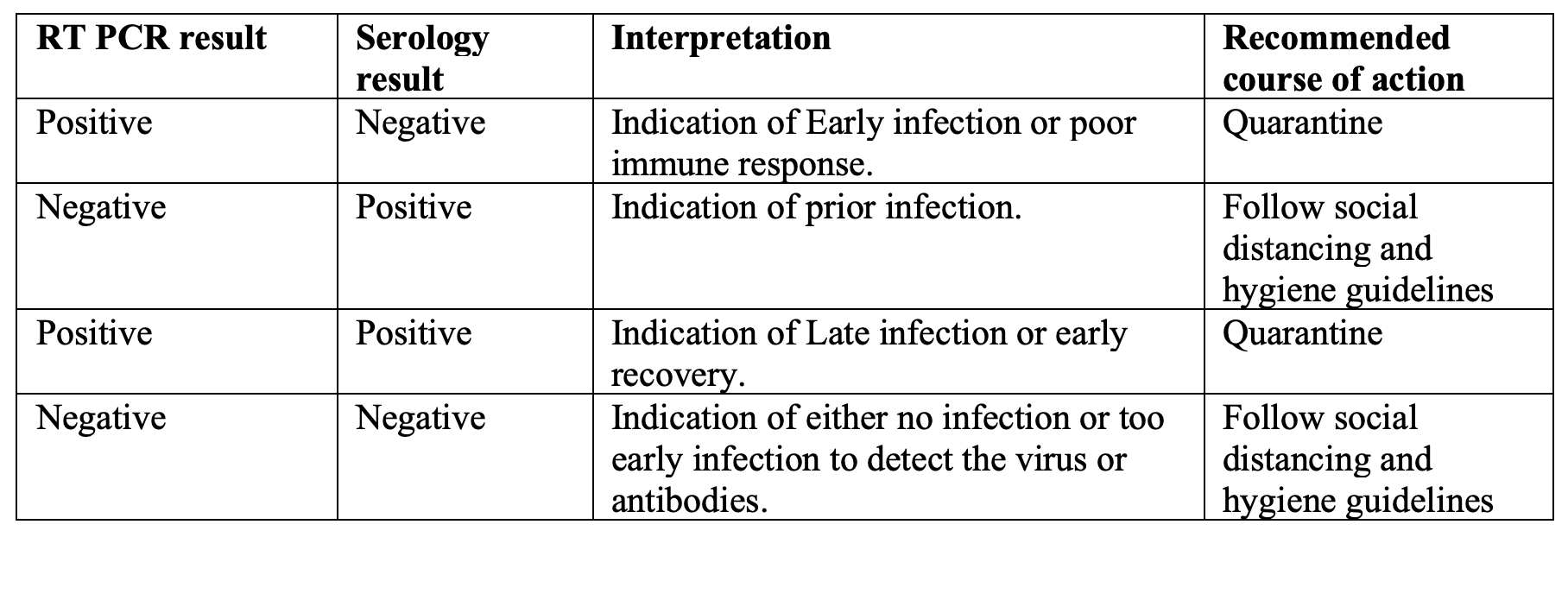
Table 2. COVID-19 Testing in Asymptomatic [10].
Summary:
In a summary is highly recommended to use both the tests for screening and confirmation of the present and/or past infection in the asymptomatic population and take the correct course of action as recommended.
References
| [1] | I. Galesburg, “COVID-19 More Contagious & Deadly than Flu,” October 02,2020. |
| [2] | W. H. Organization, “Modes of transmission of virus causing COVID-19: implications for IPC precaution recommendations,” 29 March 2020. |
| [3] | “Rt COVID-19,” Rt live. |
| [4] | A. Park, “Nearly Half of Coronavirus Spread May Be Traced to People Without Any Symptoms,” June 2020. |
| [5] | A. D. K. J. G. Alejandro Lopez-Rincon, “A Missense Mutation in SARS-CoV-2 Potentially Differentiates Between Asymptomatic and Symptomatic Cases,” WHO Bulletin, April 2020. |
| [6] | R. Wang, “Decoding Asymptomatic COVID-19 Infection and Transmission,” The Journal of Physical Chemistry Letters, November 2020. |
| [7] | L. Cella, “Injuries From Asymptomatic COVID-19 Disease: New Hidden Toxicity Risk Factors in Thoracic Radiation Therapy,” International Journal of Radiation Oncology Biology and Physics., September 2020. |
| [8] | J. Tan, “Transmission and clinical characteristics of asymptomatic patients with SARS-CoV-2 infection.,” Future Virology, May 2020. |
| [9] | L. Carter, “Assay Techniques and Test Development for COVID-19 Diagnosis,” ACS Central Science, 2020. |
| [10] | “COVID-19 Testing in Asymptomatic HCW FAQs,” Santa Clara Valley Medical Center. |
Lighthouse Lab Services offers assistance to the clinical lab industry via recruiting, consulting, and lab director services. Please, feel free to reach out to us if your lab needs any help.
Also, we operate the country’s largest members-only groups on social media. You’re welcome to join:

Very well described. Helpfull to spread good knowledge and awareness to people about SARS-COV-2 in short note.
Thank you, Anjani! Varsha did a great job with this article.
Very well said. It is true of the article because I was one of many exposed to a co-worker while in training for the job, and being “Asymptomatic” it may be my blessing, sadly not for others. I can say, I have a different prospective way of looking at life at a different angle.
People please, do take care of your ONE LIFE- YOUR ONE BODY…whether you have family or not, care enough to take extra precautions and keep safe and healthy.
Thank you for your feedback and personal experience, Jane. Keep safe and stay healthy, as well.